Last updated on February 14th, 2023 at 04:20 pm
In one of the areas of Uganda with the lowest level of resources and the lowest ratio of doctors to patients, where there is only one doctor for every 25,000 people, achievements are not ignored.
However, in the Nakaseke district of Uganda, which is approximately 65 kilometers away from the capital city of Kampala, there are three clinics that treat people with non-communicable diseases (NCDs) such as diabetes, kidney disease, and chronic lung conditions. The majority of the government health facilities in Uganda are focused on infectious diseases.
In Uganda, as in other low- and middle-income countries, the burden of illness is shifting away from tropical and infectious diseases and toward these common NCDs. These NCDs are responsible for the deaths of 41 million people every year around the world, which accounts for approximately 71% of all annual deaths worldwide.
According to the findings of a study conducted in 2021, Uganda “has been overwhelmed by the growing burden of NCDs across all socioeconomic strata.” The Balamu project’s clinics, on the other hand, have been so effective in treating patients that the Ugandan government has decided to roll out more of them across the country.
Related Posts
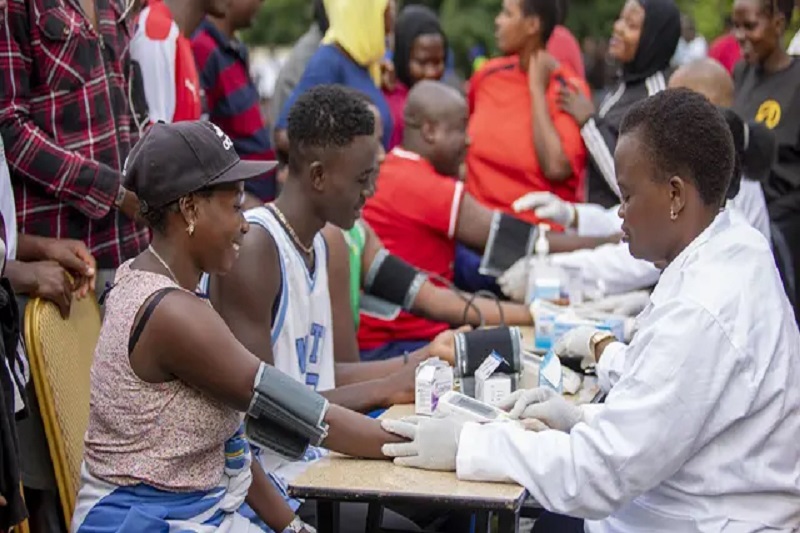
The Nakaseke general hospital’s weekly clinic is staffed by seven registered nurses and a doctor who rotates between all three of the hospital’s clinics. Every Friday, when it opens, the staff sees between one hundred and two hundred patients in a region where more than sixty percent of the population lives on less than ten pounds a month.
According to Dr. Robert Kalyesubula, founder of the African Community Centre for Social Sustainability (Access Uganda), the organization that is behind Balamu, “in Uganda, about 80% of the health worker force lives in big towns, which constitute about 20% of the population.” In other words, the majority of health workers in Uganda are concentrated in urban areas. This results in a significant disparity in the number of healthcare professionals that are on hand to attend to the needs of the vast majority of Ugandans. According to Kalyesubula, non-communicable diseases “are largely left untreated in Uganda.”
The training of health workers to assess patients, provide referrals, and follow up on medicines is an important accomplishment that has been made. They have already conducted screenings on 16,000 individuals. According to Kalyesubula, “the greatest obstacle that non-communicable diseases face in Uganda is the fact that patients pay for the majority of their care out of their own pockets, even in government facilities.”
Read More:- Burkina Faso, Guinea, and Mali all seek to rejoin regional blocs.
Research shows that only 7 percent of people with hypertension are aware that they have it, even though it is thought that between 26 and 31 percent of people have it.